Large areas of skin ulcers caused by chronic diseases such as severe burns, hemorrhoids or diabetes may one day no longer require plastic surgery. Scientists at the Salk Institute have developed a new technology that converts cells in open wounds directly into new skin cells. This approach relies on reprogramming cells into a stem-like state and may help repair skin damage, fight aging, and help people better treat skin cancer. Related research was published online in the September 5 issue of Nature.

"Our observations have constructed the entire three-dimensional tissue (such as the skin) and not just the prima facie evidence of the in vivo regeneration principle of the single cell type shown previously." Professor Juan Carlos Izpisua Belmonte, senior author of the article, said, "This knowledge will not only be Helps strengthen skin repair and guides in vivo cell regeneration strategies in other pathological conditions and during aging."
Skin ulcers - wounds can sometimes extend to multiple layers of skin - usually surgically treated to cover the wound by transplanting existing skin, however when the ulcer area is particularly large, the skin available for transplantation is often insufficient, in these cases, The doctor usually separates the skin stem cells from the patient and transplants them back into the patient after being cultured in the laboratory. However, such an operation requires a lot of time, may put the patient's life at risk, and is not guaranteed to be always effective.
Izpisua Belmonte and Salk research assistant Masakazu Kurita said that the key step in wound recovery is to transplant basal keratinocytes into the wound. These stem cell-like cells are precursors to different types of skin cells, but severe large-area ulcers lose multiple layers of skin. There is no longer any basal keratinocytes, and even if the wound eventually heals, the cells that proliferate in this area are mainly involved in wound closure and inflammation, rather than rebuilding healthy skin. Izpisua Belmonte and Kurita hope to convert these cells directly into basal keratinocytes instead of taking them out of the body. Kurita said: "We started to make skin in places where there is no skin."
The researchers first compared the different protein levels between cells involved in inflammation and keratinocytes to understand what changes they needed to reprogram cell identity. They identified 55 "reprogramming factors" (including protein and RNA molecules) that may be involved in defining the uniqueness of basal keratinocytes. Then, through repeated and further experiments on each potential reprogramming factor, the researchers narrowed the scope to four factors that could mediate conversion to basal keratinocytes.
When the research team added these four factors to treat skin ulcers in mice, the skin of the mice grew healthy in 18 days, and over time, the epithelial cells expanded and connected to the surrounding skin, even if The same is true in large area ulcers. After 3 months and 6 months, the researchers found through molecular, genetic, and cytological tests that the newly formed cells behave as healthy skin cells.
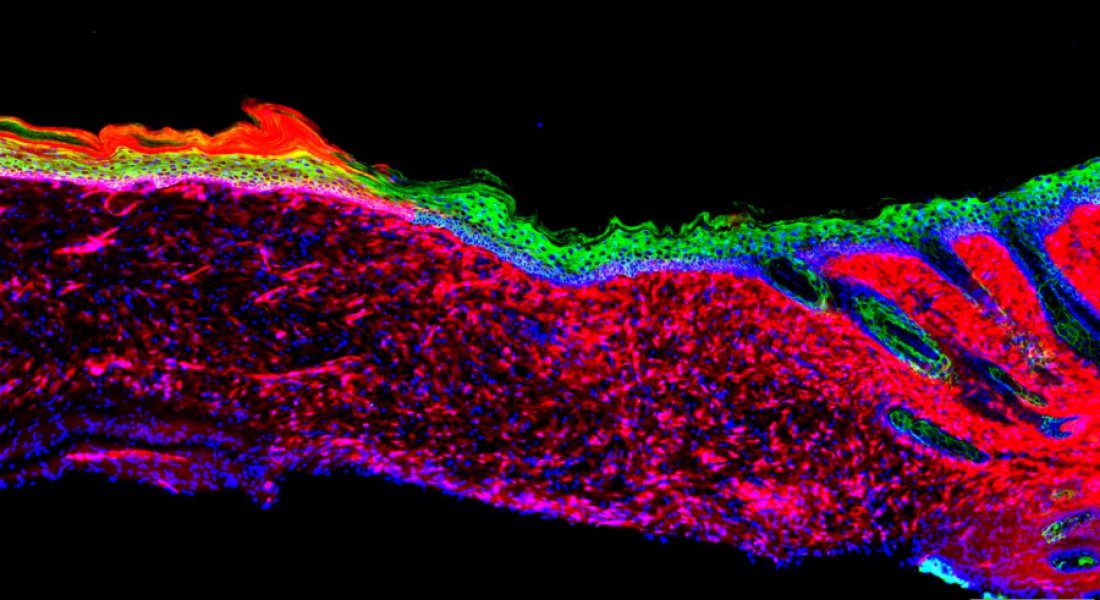
In a large-area mouse model, the researchers converted one cell type (red: mesenchymal cells) to another (green: basal keratinocytes). Credit: Salk InstituteClose
Researchers are planning more research to optimize the technology and begin testing in other ulcer models. But "Before applying to the clinic, we must do more research on the long-term safety of the method and increase efficiency as much as possible," Kurita said.
Xi'an Healthway Biotech Co.,Ltd , https://www.xianhealthway.com